Is Herbal Medicine Hepatotoxic or Hepatoprotective?
A Case of Stage IV Liver Cancer Treated with Herbal Medicine Alone
“In the previous Lecture 121, the importance of thermal therapy was discussed. Among various methods, a simple stone-heating therapy, which can be easily applied at home, was introduced. Furthermore, it was emphasized that, rather than relying on mechanical heating methods such as saunas or electric heating devices, it is preferable to use TDP therapy.”
“Sauna therapy also varies in its mechanisms. In a Finnish-style sauna, heated stones are used, and water is poured over them to produce steam, which subsequently transfers heat to the body through the skin. While these methods can enhance circulation in patients with cancer, I believe that TDP therapy remains the most favorable modality.”
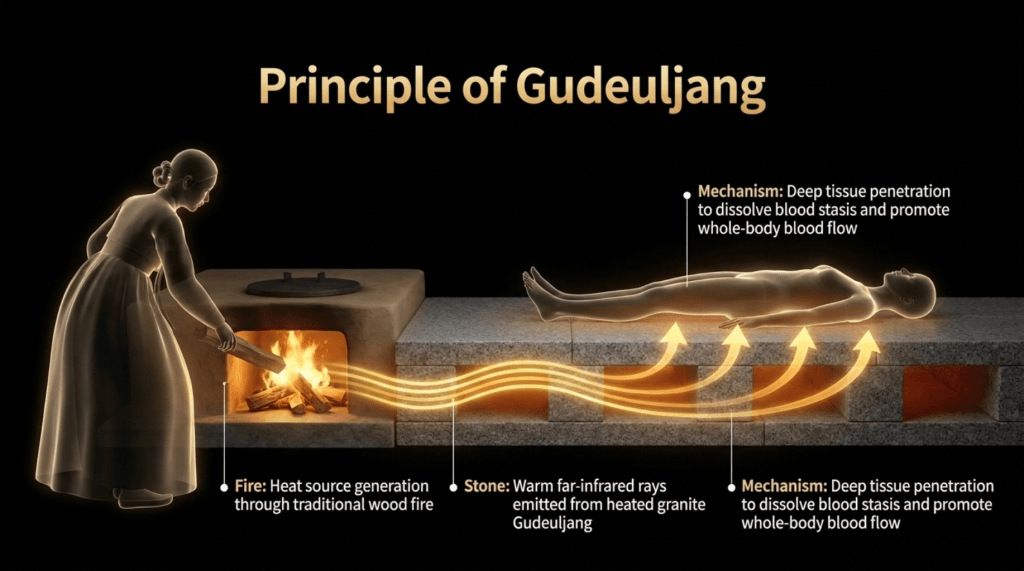
I previously visited a traditional Korean residence in Cheongsong and stayed at Songso Gotaek, a historic house nearly 150 years old. The room featured a granite-covered ondol floor system, which retained heat efficiently even with minimal firewood use. The sustained, deep warmth provided a form of whole-body thermal exposure, during which musculoskeletal discomfort noticeably diminished. Due to these effects, the site is reportedly sought out by patients seeking therapeutic benefit.



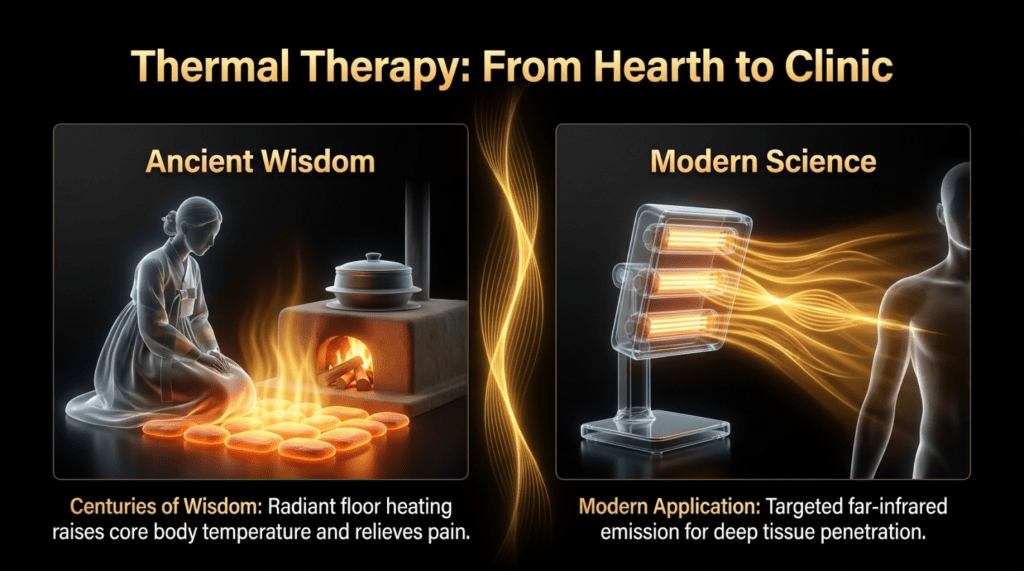
These approaches share a common underlying mechanism.
The traditional Korean agungi heating system also generates far-infrared radiation, and prolonged exposure to this thermal energy may have contributed to a lower prevalence of gynecological disorders in the past.

Today, I will present a case of a liver cancer patient who was treated using a TDP half-body thermal bath system in combination with herbal medicine, based on these principles. Although this case has been introduced previously, I will revisit it here and provide a renewed explanation.
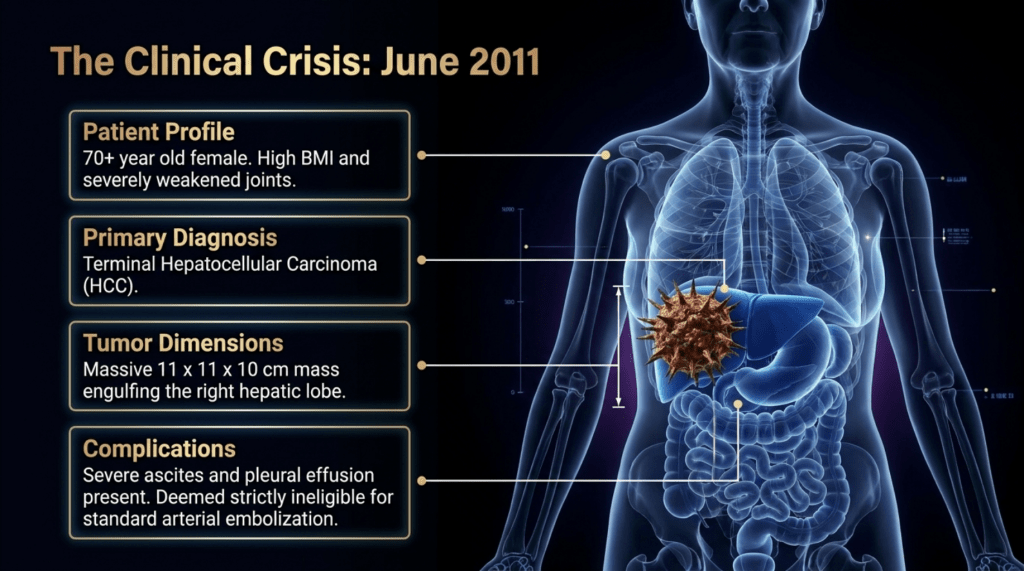

This patient was classified as a Taeeumin(Autumn type: in sasang typology) and was of advanced age. The liver cancer was detected at an advanced stage, with the right hepatic lobe almost entirely infiltrated by tumor, making transarterial chemoembolization infeasible. Sorafenib was therefore initiated. In my assessment, although sorafenib is a drug that aligns with the Taeeumin constitution, the patient experienced severe dermatologic adverse effects and discontinued the medication in less than one month.
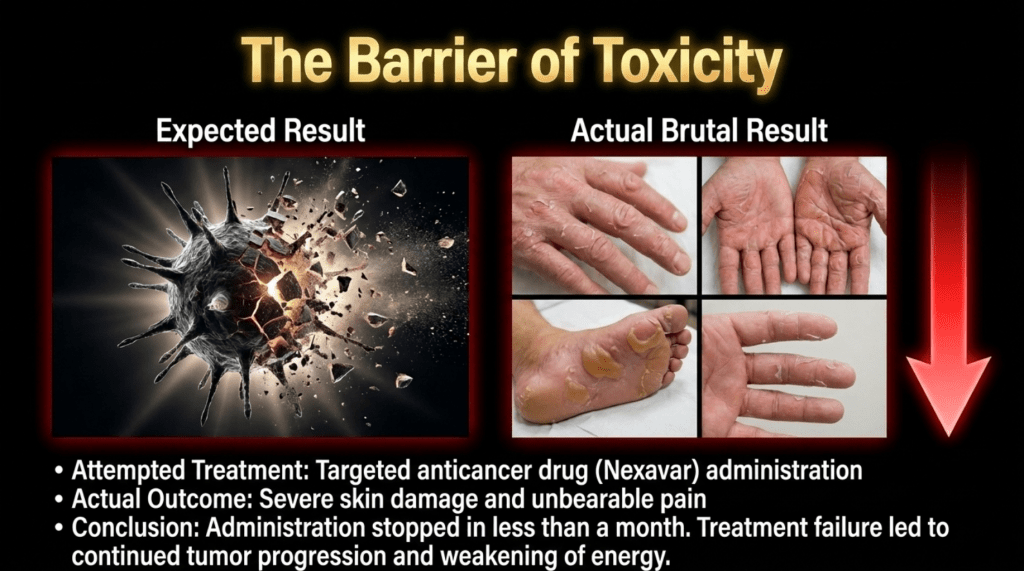
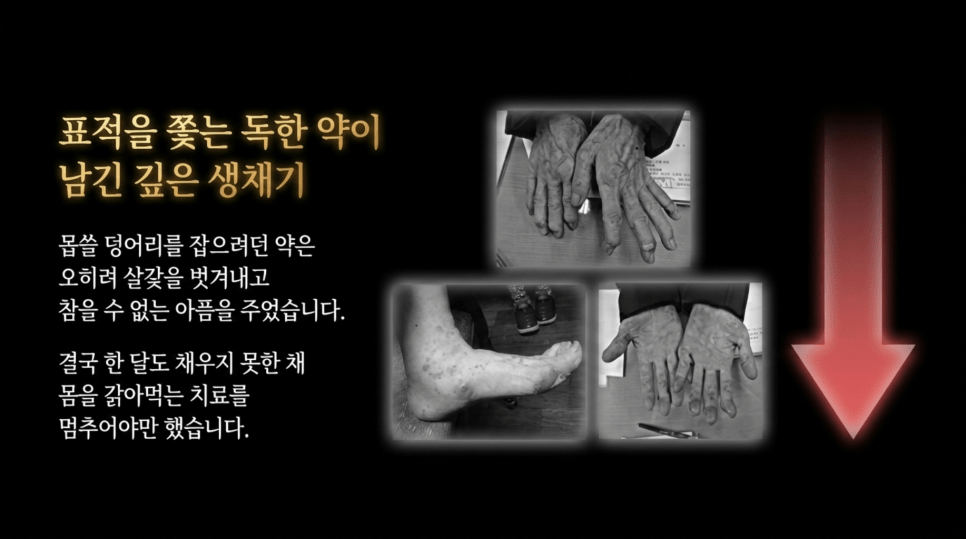
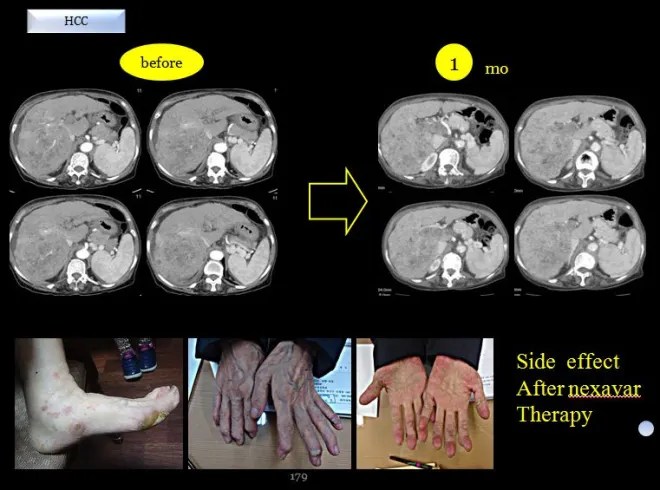
The above image shows the actual side effects observed on the patient’s hands and feet by sorafenib (Nexavar)
Previously, I encountered a Soeumin patient(winter type) who continued taking sorafenib despite severe mucocutaneous toxicity extending even to the perianal area. However, the tumor progressed very rapidly, spreading systemically and even involving the eyes.
Later, a collaborating physician requested constitutional classification, and I identified several Taeeumin patients. I was informed that, in those cases, the use of sorafenib led to very favorable outcomes. However, in this particular patient, severe dermatologic adverse effects affecting the hands and feet made continued use impossible, leading to discontinuation and subsequent presentation to my clinic.
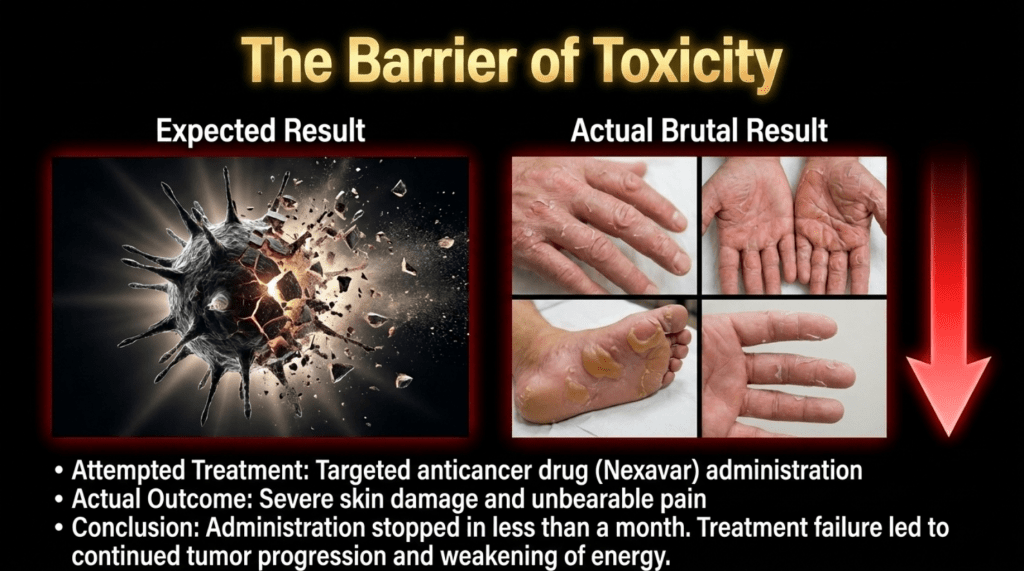
As shown above, after approximately one month of sorafenib use, the tumor had progressed further, and there was extensive peeling of the skin on the hands and feet. The patient was over 70 years old, and at that time had severe ascites and pleural effusion. In my assessment, the prognosis appeared very poor, and survival was expected to be limited.
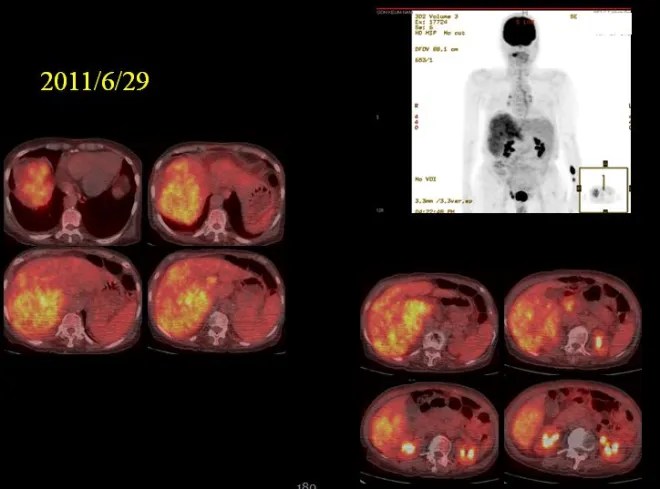
As seen on the PET scan, the entire right hepatic lobe was involved by tumor. I therefore explained my perspective to the family. If the patient were younger, I would consider attempting treatment, and some prolongation of survival might be expected. However, given the current condition—with both pleural effusion and ascites requiring albumin supplementation, and the likelihood of repeated hospital visits for paracentesis and supportive care—it would place a significant burden on both the patient and the family. In today’s busy circumstances, this can be especially difficult, and in such an elderly patient, I explained that a more conservative, comfort-oriented approach might ultimately be more appropriate.
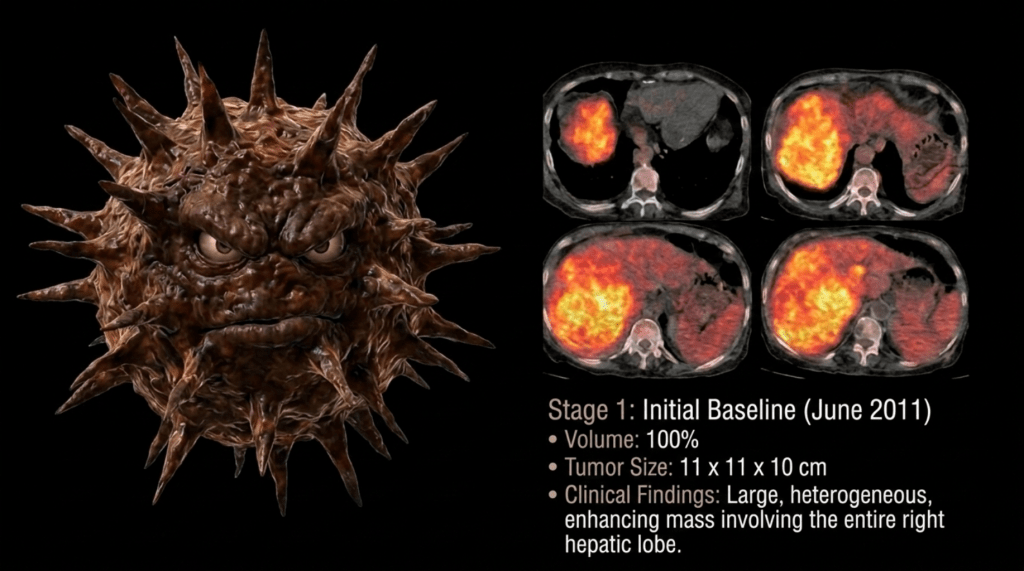
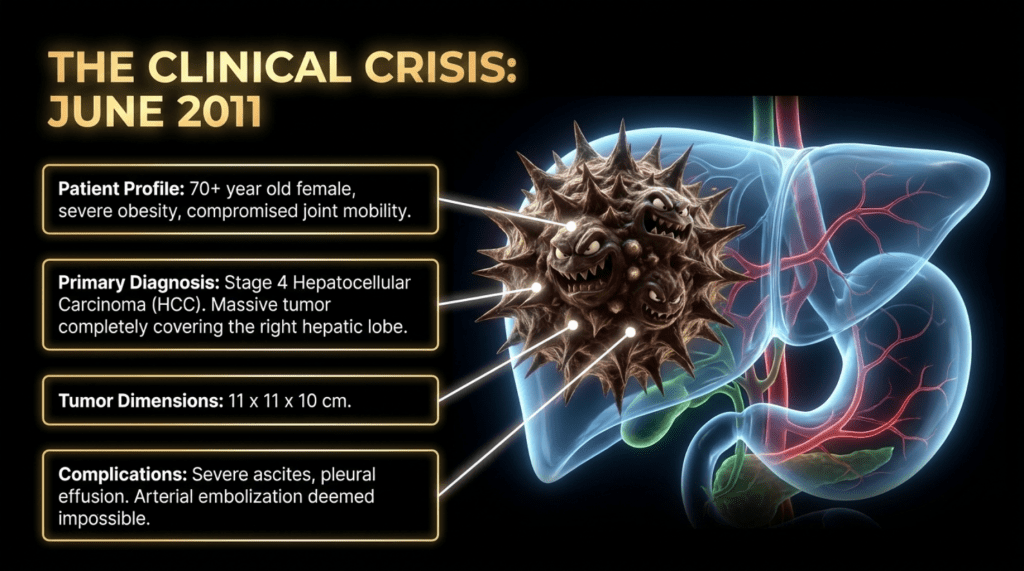
Although this may sound harsh to the patient and family, I believed that attempting to prolong survival with herbal medicine would likely impose a significant burden, and from the perspective of quality of life, it would be extremely difficult.
However, the patient’s children showed remarkable devotion and a strong sense of family unity. They explained that their mother had raised them through great hardship, working in the marketplace to support their education, and that they felt a deep responsibility to repay her. They expressed their determination to do their very best, regardless of the physical and financial difficulties involved.
The patient was overweight, had weak knees, and was obese, making it unlikely that she would be able to engage in exercise or other supportive therapies typically recommended for general patients.
Therefore, a TDP thermal therapy device was set up at home, and the patient was instructed to undergo heat therapy in the morning and evening while taking herbal medicine. Since sorafenib, although constitutionally suitable for Taeeumin, could not be continued due to severe adverse effects, treatment was initiated with herbal medicine alone.
Remarkably, the ascites gradually resolved, and the patient was able to maintain her condition and survive for more than three years.
Ascites is generally not easily resolved with medication alone. As discussed in Lecture 121, it is thought that the far-infrared radiation generated by radiant heat may have contributed to this effect.
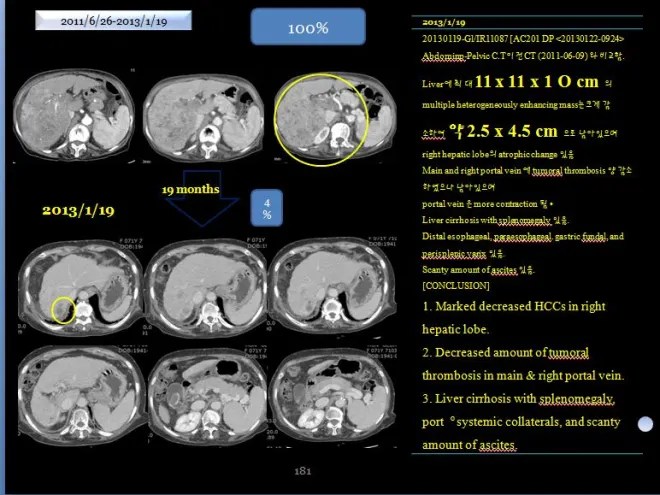
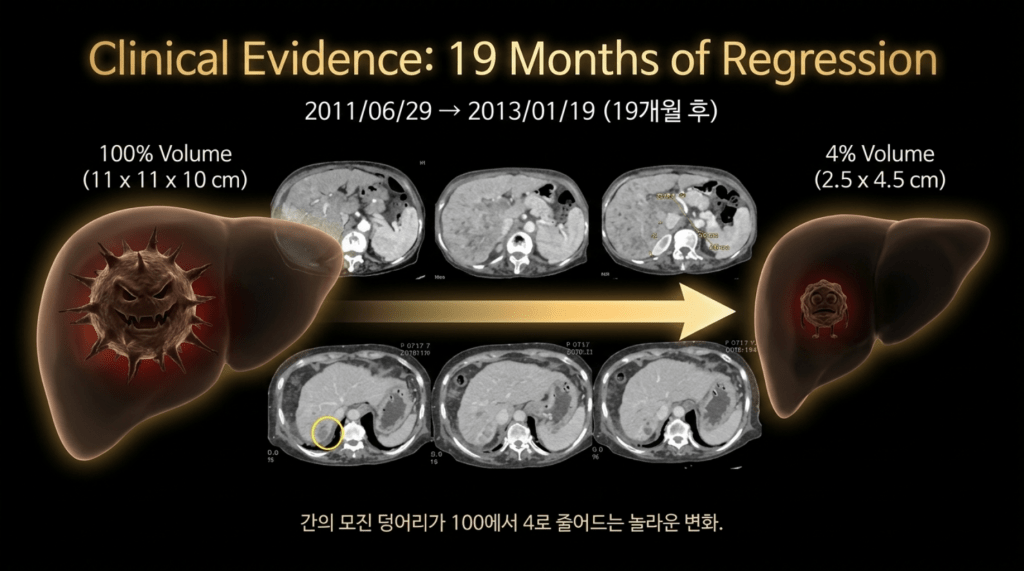
The patient was able to tolerate the course well for nearly two years, with both ascites and pleural effusion resolving, allowing a return to normal daily activities. The CT scan obtained 19 months later showed the findings as above.
As seen in the imaging, the liver had become atrophic; however, the large tumor had almost completely regressed, with only a small residual portion remaining. The medical records at that time documented the following findings.
- 20130119
- Abdominp-Pelvic C.T 이전 CT (2011-06-09)와 비교함.
- A previously noted multiple heterogeneously enhancing mass in the liver, measuring up to 11 × 11 × 10 cm, has markedly decreased in size, with a residual lesion measuring approximately 2.5 × 4.5 cm. Atrophic changes of the right hepatic lobe are also observed.
- Main and right portal vein에 tumoral thrombosis 양 감소하였으나 남아 있으며
- portal vein은 more contraction 됨.
- Liver cirrhosis with splenomegaly 있음.
- Distal esophageal, paraesophageal, gastric fundal, and perisplenic varix 있음.
- Scanty amount of ascites 있음.
- [CONCLUSION]
- Marked decreased HCCs in right hepatic lobe
- Decreased amount of tumoral thrombosis in main & right portal vein
- Liver cirrhosis with splenomegaly, port。systemic collaterals, and scanty
- amount of ascites


“Comparison of CT scans from June 9, 2011 and January 19, 2013 shows that the previously noted heterogeneously enhancing hepatic tumor, measuring up to 11 × 11 × 10 cm, has markedly decreased in size to approximately 2.5 × 4.5 cm. The right hepatic lobe demonstrates atrophic changes. Tumor-related thrombosis in the main and right portal veins has decreased but remains present, and the portal vein appears further narrowed. Findings of liver cirrhosis and splenomegaly are noted. Varices are observed adjacent to the spleen around the esophagus and stomach, and a small amount of ascites is present.
Within 18 months, the hepatic tumor had decreased to approximately 4% of its original volume. In March 2014, I was invited to present at the Korea–China–Japan Integrative Medicine Conference, and in preparation for this presentation, I recommended that the patient undergo a follow-up CT scan after about one year.
The patient lived in Jeolla Province, quite far away, and had not visited frequently, instead receiving prescriptions and consultations by phone. Given her stable condition, repeated CT imaging had not been performed regularly.
She resided in Gwangju and continued treatment primarily through remote consultation and consistent use of prescribed herbal medicine. By the spring of 2014, more than three years into the course, the tumor had further decreased in size; however, there were partial findings suggestive of recurrence.
In general, there is considerable skepticism in Korea regarding the role of Korean medicine in cancer treatment.
In this case, while practitioners of traditional medicine (sasang typology medicine) may find the results credible, others may remain doubtful. Therefore, I will present the medical records as they are.AI usage settings
Please enter an image description.

Abdomen–Pelvic CT (Dynamic)
Follow-up for HCC
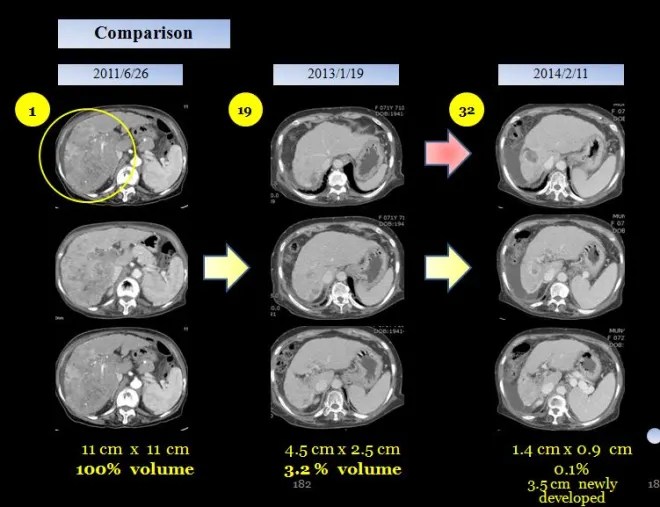
Comparison with previous CT (January 19, 2013):The previously noted multiple heterogeneously enhancing hepatic masses have decreased from 2.5 × 4.5 cm to 1.4 × 0.9 cm.
Atrophic change of the right hepatic lobe is again noted.
A newly developed 3.5 cm heterogeneously enhancing mass is observed in segment 8 of the liver.
Tumoral thrombosis in the main and right portal veins has further decreased compared to the previous study, although residual thrombosis remains, and the portal vein shows further contraction.
Liver cirrhosis with splenomegaly is present.
Distal esophageal, paraesophageal, gastric fundal, and perisplenic varices are noted.
A small to moderate amount of ascites is present.No significantly enlarged lymph nodes are observed around the aorta and IVC.
Both kidneys show small cysts.
Gallbladder is unremarkable.
No remarkable findings in the pancreas.
Conclusion:
Further decrease in size of previously noted HCCs in the right hepatic lobe.
Newly developed 3.5 cm HCC in segment 8 of the liver.
Decreased extent of tumoral thrombosis in the main and right portal veins.
Liver cirrhosis with splenomegaly, portosystemic collateral vessels, and small to moderate ascites.
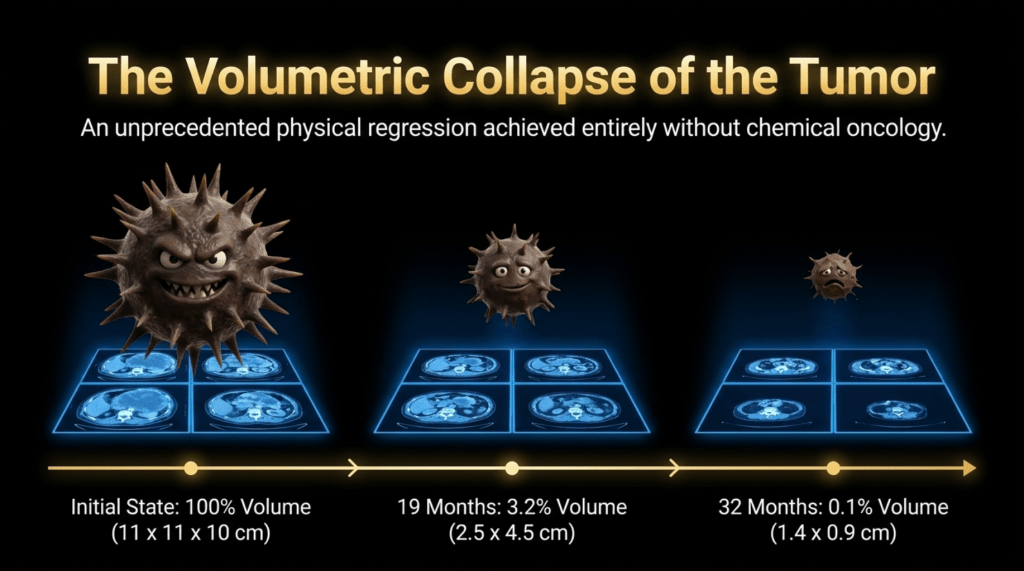

By February 2014, the patient’s tumor burden had nearly resolved. The previously existing tumor had decreased to approximately 0.1% of its original size compared to baseline. However, a newly developed 3.5 cm lesion was identified in another region. After this point, the patient did not receive further treatment.
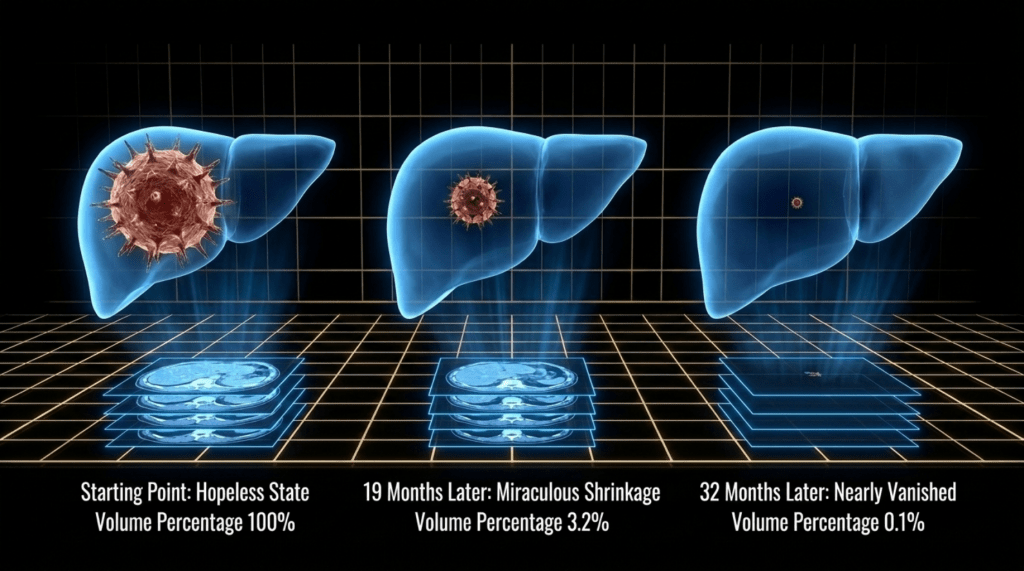
After discontinuing herbal medicine, approximately nine months later, as winter approached, the patient’s physical strength declined, ascites recurred, and hepatic function deteriorated, ultimately leading to death. At that time, the patient did not return for follow-up and had already stopped taking the herbal medicine, so the exact clinical course during that period could not be fully assessed.
However, considering that this patient, even in the terminal stage, was able to maintain daily life for over three years with marked tumor reduction, the contributing factors can be summarized into three main points.
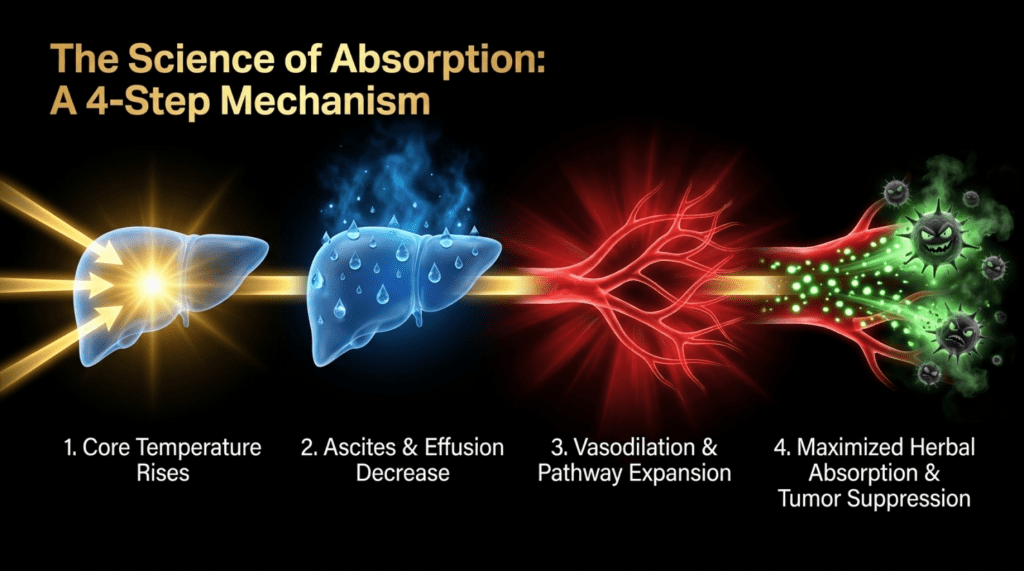
First, the herbal medicine itself had therapeutic efficacy. However, without sufficient physical strength, absorption would be limited, and the treatment effect would not be adequately achieved. In this case, it is thought that TDP therapy contributed to the reduction of ascites and pleural effusion, increased effective blood volume, and thereby improved the absorption and overall effectiveness of the herbal treatment.
Finally, and perhaps most importantly, the patient was supported by devoted family members—two sons and daughters-in-law—who provided unwavering care and dedication. This level of familial support likely played a critical role in sustaining the patient’s condition and prolonging life. Without such support, it is unlikely that medication alone would have achieved this outcome.


Furthermore, this case demonstrates that, even without the aid of conventional Western medicine, a tumor that had occupied nearly the entire liver regressed significantly with herbal medicine alone, allowing the patient to survive for almost four years. Although complete cure was not achieved, this outcome remains highly meaningful.
Based on such results, it is necessary for Western medicine to recognize and further investigate constitution-based therapeutic approaches, such as those in Sasang medicine, in order to improve treatment outcomes and reduce patient suffering through an integrative medical framework.
It is often casually stated that herbal medicine is toxic and harmful to the liver. However, in this case, it was rather the conventional drug that caused severe adverse effects, including extensive skin peeling, and was associated with rapid tumor progression, yet such concerns are not emphasized in the same way.
From this case, it can be observed that herbal medicine—often assumed to be hepatotoxic—actually contributed to maintaining life for an additional three years in a terminal-stage liver cancer patient. This suggests that herbal medicine is not inherently harmful to the liver, but may instead have therapeutic benefits.
The key issue lies in appropriate patient-specific application. Matching treatment to individual constitution is not easily achieved in general clinical settings, which may explain why such outcomes are relatively rare.
Nevertheless, this case illustrates that when properly aligned with the patient’s constitutional characteristics, herbal medicine may offer therapeutic potential even in liver cancer cases considered untreatable by conventional medicine.
======================================================================
📘 Title
Long-term Survival and Tumor Regression in a Stage IV Hepatocellular Carcinoma Patient Treated with Herbal Medicine Alone and TDP-Based Thermal Therapy: A Case Report
📖 Abstract
This case report describes a patient with advanced hepatocellular carcinoma (HCC) who demonstrated significant tumor regression and prolonged survival following treatment with herbal medicine alone in combination with TDP-based thermal therapy.
The patient, diagnosed with stage IV HCC involving extensive right hepatic lobe infiltration, was not eligible for transarterial chemoembolization and discontinued sorafenib due to severe adverse effects.
Following initiation of herbal medicine and home-based TDP thermal therapy, ascites resolved, functional status improved, and the patient survived for more than three years. Imaging studies revealed a marked reduction in tumor size to approximately 4% of the original volume within 18 months.
This case suggests a potential role of individualized herbal medicine and thermal therapy in advanced HCC, particularly in patients intolerant to conventional treatment.
📖 Introduction
Hepatocellular carcinoma remains a major cause of cancer-related mortality worldwide, especially in advanced stages where treatment options are limited.
Although systemic therapies such as sorafenib have demonstrated survival benefits, their use is often restricted by adverse effects and limited tolerability in elderly patients.
Traditional Korean medicine, including herbal therapy and thermal interventions, has been explored as an alternative or complementary approach; however, clinical evidence remains limited.
This report presents a case of stage IV HCC treated with herbal medicine alone combined with TDP-based thermal therapy, demonstrating significant clinical and radiologic improvement.
📖 Introduction
Hepatocellular carcinoma remains a major cause of cancer-related mortality worldwide, especially in advanced stages where treatment options are limited.
Although systemic therapies such as sorafenib have demonstrated survival benefits, their use is often restricted by adverse effects and limited tolerability in elderly patients.
Traditional Korean medicine, including herbal therapy and thermal interventions, has been explored as an alternative or complementary approach; however, clinical evidence remains limited.
This report presents a case of stage IV HCC treated with herbal medicine alone combined with TDP-based thermal therapy, demonstrating significant clinical and radiologic improvement.
📖 Case Presentation
A female patient over 70 years of age, constitutionally classified as Taeeumin, was diagnosed with advanced HCC.
At initial presentation in June 2011, imaging studies revealed extensive tumor involvement of the right hepatic lobe, rendering transarterial chemoembolization infeasible. Sorafenib was initiated but discontinued within one month due to severe dermatologic toxicity.
At that time, the patient exhibited severe ascites and pleural effusion, with poor functional status and an expected limited prognosis.
Treatment was initiated using herbal medicine alone, combined with twice-daily TDP-based thermal therapy at home.
📖 Treatment
Herbal medicine tailored to constitutional characteristics
TDP (far-infrared) thermal therapy applied morning and evening
No continuation of conventional systemic chemotherapy
📖 Results
Clinical Outcomes
Resolution of ascites and pleural effusion
Improvement in daily functional activity
Survival exceeding 3 years
Radiologic Outcomes
Initial tumor size: 11 × 11 × 10 cm (maximum diameter)
At 19 months (January 2013):
Residual lesion: approximately 2.5 × 4.5 cm→ Estimated tumor volume reduction to approximately 4% of baseline
Additional findings:
Right hepatic lobe atrophy Reduced portal vein tumor thrombosis Persistent cirrhosis and splenomegaly At February 2014 follow-up CT:
Further reduction of previous lesions Newly developed 3.5 cm lesion (segment 8)
Continued decrease in portal vein thrombosis Small to moderate ascites
📖 Discussion
This case demonstrates an unusually prolonged survival and significant tumor regression in a patient with advanced HCC treated without conventional systemic therapy.
The mechanisms underlying this outcome may include:
Immunomodulatory effects of herbal medicine
Improvement in microcirculation through thermal therapy
Enhanced lymphatic flow and metabolic regulation
Individualized treatment based on constitutional characteristics
TDP therapy emits far-infrared radiation, which may penetrate tissue and promote circulation, potentially contributing to ascites resolution and improved hepatic function.
It is notable that tumor reduction occurred despite discontinuation of sorafenib, suggesting that non-conventional interventions may have played a significant role.
However, this is a single case, and conclusions regarding efficacy must be interpreted with caution.
📖 Limitations
Single case report
Lack of control group
Potential selection bias
Mechanistic pathways not directly validated
📖 Conclusion
This case suggests that herbal medicine combined with TDP-based thermal therapy may provide clinical benefit in selected patients with advanced hepatocellular carcinoma, particularly those who are unable to tolerate conventional treatment.
Further studies are required to validate these findings and elucidate underlying mechanisms.